Congratulations, mama! You survived TEN grueling months of nausea, swollen ankles, frequent urination, and sleep deprivation. Your reward? A tiny, adoring human — and the return of your monthly visitor. While you are thrilled to be a mother, you’re not quite ready to do it again – at least not in the near future . . .
Or maybe your tiny human isn’t so tiny anymore, but your flow is heavy, your period cramps and mood swings are unbearable, and you just can’t take it anymore . . .
Perhaps your family is complete, but your ovaries haven’t gotten the message . . .
Or maybe you don’t believe in birth control, but still want to manage your fertility . . .
Or maybe certain contraceptive methods do not agree with your body . . .
The reasons for choosing to start birth control vary widely and are incredibly personal. The options are diverse and can be a little confusing. So let’s talk about birth control, or fertility management, or relief of painful menstruation, or whatever it is for you.
Fertility Cycle
To understand contraception, we have to discuss the physiology of our menstrual cycle and pregnancy. We are incredibly complex, so bear with me:
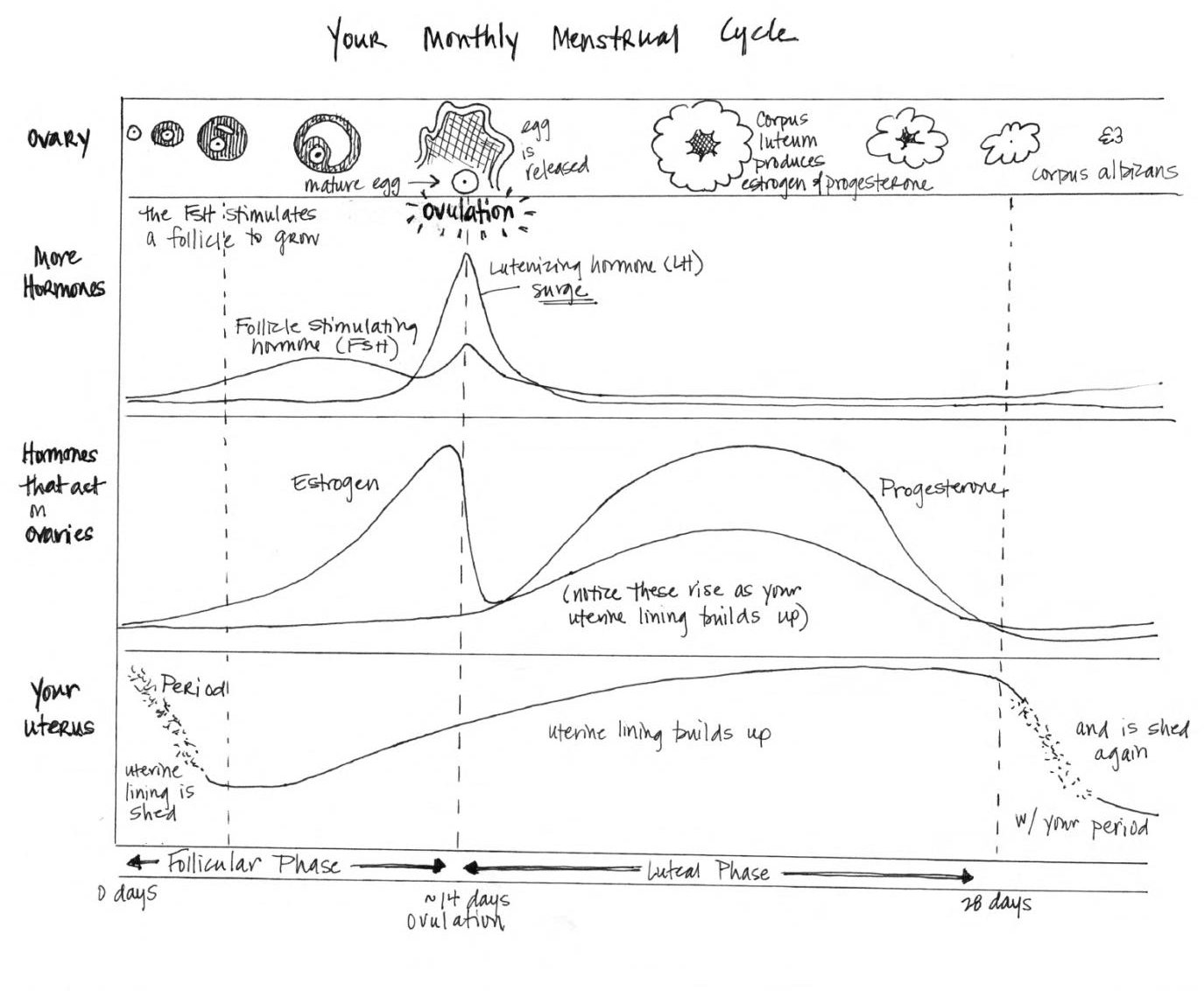
We say “monthly period.” But in reality? Cycle lengths vary from roughly 23-35 days. The first day of your period is cycle day 1. There are two parts to this cycle: t he follicular phase (where the egg matures in the follicle, which lasts roughly 14-21 days) and the luteal phase (which begins with the release of this egg – ovulation – and ends with your next period).
So, your cycle starts with your period, which typically lasts 3-7 days. During this time, hormones cause you to shed the lining of your uterus.
We joke about being “hormonal,” but there are FOUR (potentially FIVE!) hormones at play during this cycle. Did I mention we are complex?
- Follicle Stimulating Hormone (FSH) – this hormone is released by the pituitary gland in your brain. While you are getting your period, the levels of FSH gently rise to stimulate the follicles in your ovary. These follicles produce another hormone, estrogen, which increases as you move toward ovulation (around day 14).
- Estrogen – thickens the lining of the uterus with nutrients and blood (which would support the growth of a fertilized egg). Estrogen also thins the cervical mucous, making it easier for the sperm to swim toward the egg. You may notice a thinner, more slippery, white discharge as you near ovulation (around day 14).
- Luteinizing Hormone (LH) – stimulates the release of the egg from the ovary
- Progesterone – builds up the lining of the uterus (after ovulation)
- Human Chorionic Gonadotrophin (hCG) – the pregnancy hormone
Ok, so in the past 14 (or so) days you’ve bled, then stopped, and your FSH hormone has worked its magic in your ovaries to stimulate the growth of one dominant follicle. Within this follicle, an egg has been maturing. Your estrogen levels have been rising, which causes a very rapid increase in luteinizing hormone (an LH surge) – which causes that follicle to rupture and release the egg into the Fallopian tube. Bam, you just ovulated.
Fun Fact: ovulation kits measure this LH surge to let you know that an egg will be released soon. If you’re trying to get pregnant, this is the ideal time to have sex.
And now, another hormone enters the game: progesterone. Like estrogen, this hormone causes the lining of your uterus to build up further, to prepare for a fertilized egg. While the uterine lining is building up, the ruptured follicle continues to produce progesterone as well as estrogen. We can blame this combo for our PMS symptoms.
If the egg is not fertilized, the amount of estrogen and progesterone from that ruptured follicle decreases. Since these hormones were working to build up the uterine lining, their decrease triggers a breakdown of the lining, and your body sheds the lining on day 1 of your next cycle, this is your period.
If the egg IS fertilized, congrats mama! The egg would then (hopefully) implant into the uterus about a week later, and your body begins to produce human Chorionic Gonadotrophin (hCG), the pregnancy hormone.
Fun Fact: When you take a home pregnancy test, you are testing for the presence of hCG.
The hCG hormone acts on the ruptured, empty follicle to keep it active and producing the estrogen and progesterone hormones which support the uterine lining, and keep it from being shed (which is why your period stops).
Whew! That’s pretty amazing isn’t it?
Stay tuned for Part 2: Family Planning Options and How They Work . . .